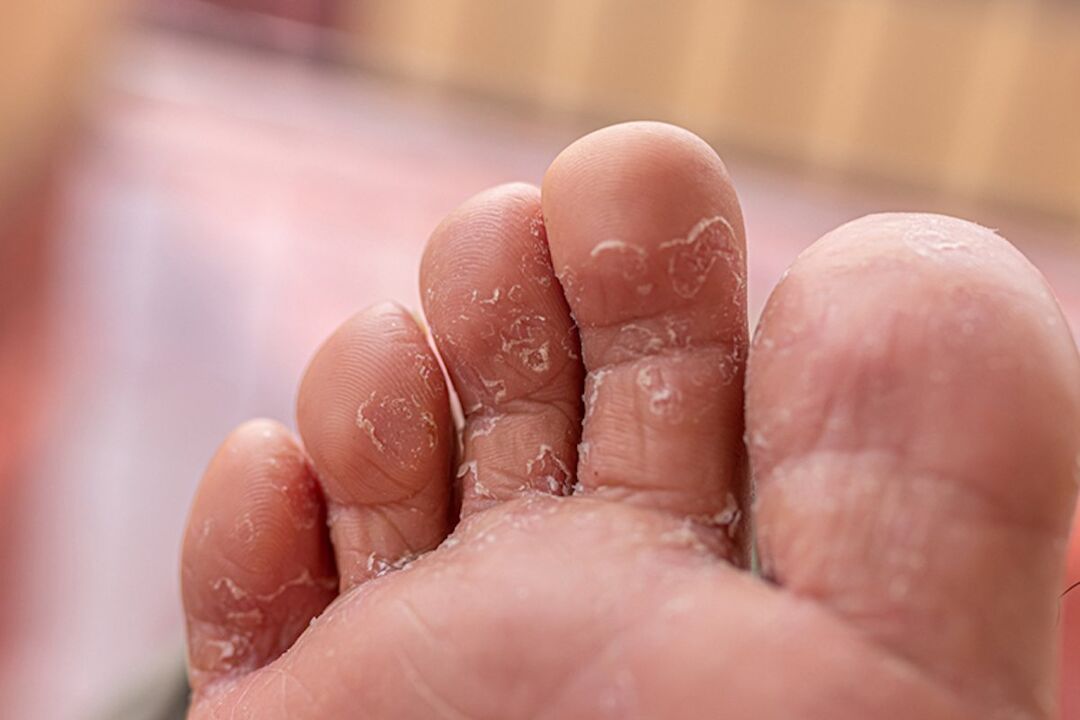
Interdigital mycoses is a fungal infection of the skin in the spaces between the fingers, the causative agents of which are opportunistic organisms and anthropophilic fungi.
Causes of fungal diseases
The cause of any fungal disease is contact with an infected person, wearing shoes or sharing toiletries with that person. The likelihood of infection increases in people with impaired immunity - due to chronic diseases, taking certain medications or due to vitamin deficiency.
At risk are patients with:
- dysfunction of the endocrine system;
- diabetes and its complications (especially diabetic foot);
- atopic dermatitis;
- varicose veins;
- fat;
- increased sweating;
- immune disorders;
- Hormonal disorder;
- metabolic disorders in the body, etc. v.
The skin on the feet after cutting toenails is very susceptible to fungus. And wearing shoes that are too tight can significantly aggravate the situation.
Symptom
Interdigital toenail fungus in the early stages is manifested by mild itching of the skin between the toes. After that, this symptom causes skin peeling, redness and cracks to appear.
If you do not take action and consult a specialist, the problem will gradually worsen - burning, diaper rash and swelling between the fingers will appear. Small, easily agglutinated bubbles may begin to form in the creases between the fingers. When such bubbles burst, the erosions remain in their place and are covered by a crust. This condition is dangerous due to infection - the wound can fester.
It is important to note that with a long period of interdigital mycosis, forms of the disease can transform into each other or develop in parallel.
Interdigital mycosis can also occur in an erased form - in this case, the patient periodically experiences unpleasant symptoms of the disease (usually during and after underwater procedures and sweating of the feettoo much).
Diagnosis of fungus between the toes
As practice shows, in about a third of cases of skin lesions between the toes, a fungal infection is diagnosed.
When prescribing treatment for fungal diseases, the specialist will take into account many factors: the presence or absence of concomitant pathologies in the patient, the clinical picture of the disease, its form and severity.
Diagnosing the specific pathogen is key to effective treatment and successful recovery. To determine which fungus needs to be fought, the podiatrist may order the patient laboratory tests and bacterial cultures.
How to treat interdigital thrush?
For interdigital mycosis, complex therapy is carried out. It includes:
- topical antifungals (creams, lotions, ointments, etc. );
- Oral antifungal medications can also be used.
The course of treatment is determined individually for each patient. Traditional medicine (compresses, baths, lotions from medicinal plants, etc. ) can be used as an auxiliary method, but only after consulting a specialist.
If mycosis develops based on internal diseases, local therapy is combined with treatment of the underlying pathology.
Contraindications and possible complications may occur
Interdigital mycosis requires referral for specialized and complex therapy. If not treated promptly, the disease will quickly spread to the entire foot and affect the nails.
In addition, in patients with fungal diseases, the body's susceptibility to viral diseases increases, the risk of bacterial infections and allergic reactions also increases.
Strict adherence to the podiatrist's recommendations and complete course of treatment are very important. Pathogens can become resistant to the drugs used and associated with repeated infections, which makes it much more difficult to eliminate the infection - even with positive momentum, the treatment processTreatment cannot be interrupted.
Advice and recommendations from a podiatrist
To avoid fungal infections, it is necessary to strictly follow the rules of personal hygiene - first of all, this applies to personal hygiene items and shoes.
- Don't wear other people's shoes and only use your own towel.
- Do not walk barefoot in the bathroom, sauna or swimming pool - this is the ideal environment for fungus to grow because it is always warm and humid.
- If you experience excessive sweating on your feet, you should consult a podiatrist about using antiperspirants.
- Avoid wearing shoes that are too tight and avoid synthetic socks and stockings as they do not allow the skin to "breathe".
To care for the skin of the feet, podiatrists recommend giving preference to hardware methods of care - trimmed toenails are today considered outdated and unsafe. It is difficult to control how to handle toenail clippers - the risk of infection increases significantly. With a hardware pedicure, the possibility of infection will be eliminated.



























